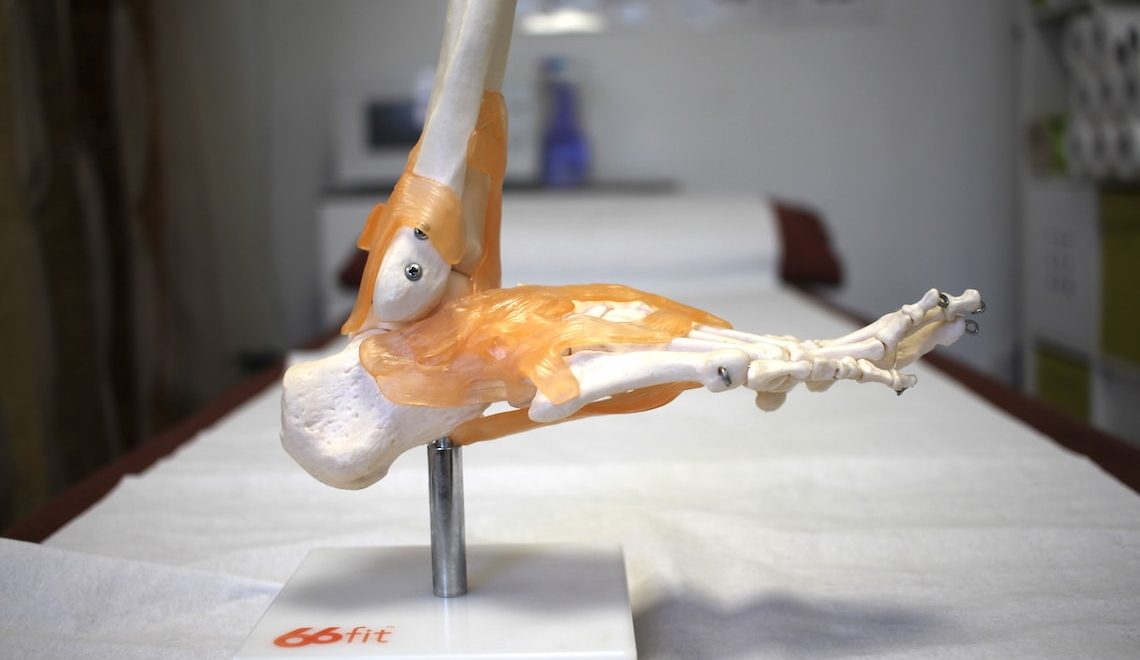
Plantar fasciitis often felt as heel pain, is an overuse injury that affects the plantar fascia on the sole of the foot. The plantar fascia is a tough, fibrous band of tissue that connects your heel bone to the base of your toes. The plantar fascia provides support to the arches of your foot. When this tissue degenerates or becomes inflamed, it is referred to as Plantar Fasciitis or Policeman’s Heel.
Symptoms
Plantar fasciitis normally starts gradually, with mild tenderness at the heel. You will begin to feel discomfort after, rather than during activity. But as the condition progresses, your pain will increase limiting your ability to walk or stand for long periods.
Here are the top 7 symptoms:
- Pain that is located on the sole of the foot, normally just in front of the heel;
- Discomfort that is stabbing or burning in nature;
- Symptoms are worse in the morning;
- Prolonged walking causes pain;
- Standing aggravates symptoms;
- Discomfort when stretching the sole of the foot;
- Tenderness when touching the base of the foot
It’s important that you treat plantar fasciitis, and to do so quickly. If left, it can become a chronic longterm condition, leaving you being unable to continue your normal sports and activities. Foot and heel pain will also cause changes in your posture, these changes can result in back, hip and knee pain.
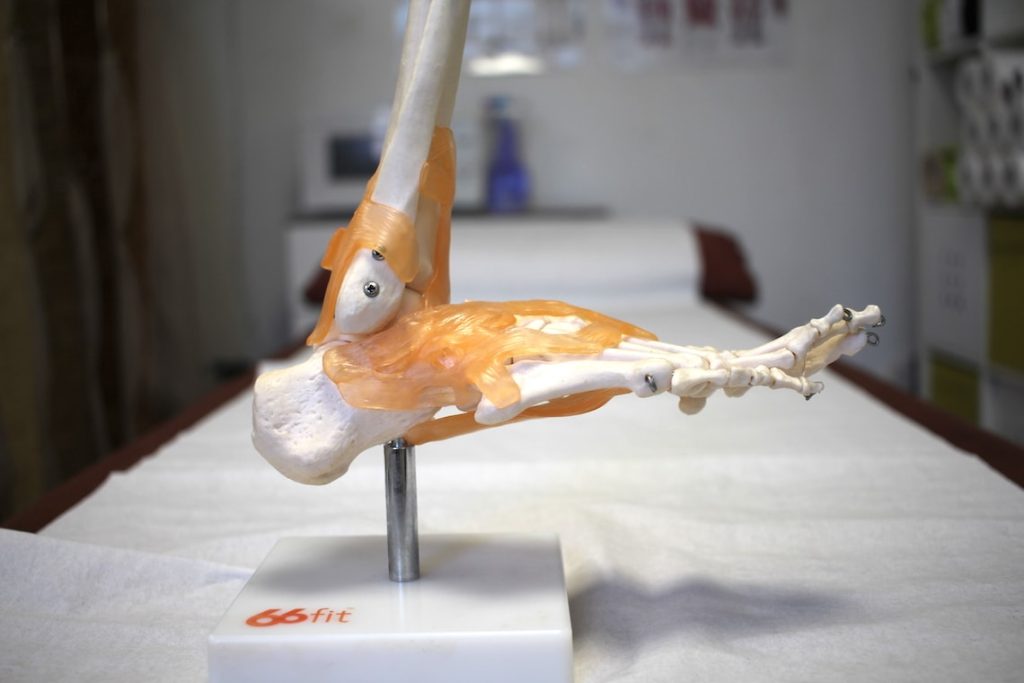
Causes
Plantar fasciitis is caused by tiny tears forming in the strong band of fascia (the plantar fascia) that supports your foot. These tears occur after repeated stress and strain to the arches of your foot. Over time inflammation and degeneration of the tissue occurs, this is what causes you to feel pain. The factors that can predispose you to developing plantar fasciitis include:
Too much physical activity – Plantar fasciitis is common in runners, walkers and in those who are on their feet all day. These activities stress the plantar fascia and surrounding tissues, especially if these activities are performed for prolonged periods and frequently.
Diabetes – Plantar fasciitis occurs more frequently in people with diabetes, this could be due to reduced neurological and vascular supply to the foot. It can be associated with diabetic foot, another complication associated with diabetes.
Poor foot mechanics – Over-pronating, having flat feet or high arches can all result in extra stress and strain on the plantar fascia.
Overweight – Being overweight puts extra strain on the arches of the feet.
Age – As you age the arches of the feet begins to sag, putting increased stress on the plantar fascia.
Arthritis – Some rheumatic disorders can cause inflammation in the tendons and other soft-tissues in your body. In some cases this can include the feet, resulting in plantar fasciitis.
Prevention
When your participating in sporting of physical activities, always think “FITT”:
- Frequency – how often you exercise;
- Intensity – how intense and physically demanding the exercise is;
- Type – the type of exercise i.e. swim, run, weights;
- Time – how long your workouts are.
Try not to increase more than one of the above FITT at any one time. When you do increase, say the Frequency of your activity; wait 3-4 weeks before extending the length of Time you spend doing that activity. This allows your body and its tissues time to adapt to the increased demand.
Plantar fasciitis treatment
It’s important to note that the plantar fascia heals slowly, on average 6–12 weeks for pain to subside. However there are a number of things that you can do to speed up your recovery.
Rest – It’s important to rest any injured area as much as possible. Activities that are aggravating to your condition should be avoided or limited as much as possible. Avoid running, long walks and over stretching. Gentle walking should not aggravate your condition and should help to maintain range of movement and strength.
Ice – Apply ice to your painful area (not directly to the skin) for 10 minutes three times a day, to relieve pain and inflammation. One popular option is to freeze a small bottle of water and then roll/massage this along the sole of the foot.
Taping – As full rest is not always possible, taping can give good support to the plantar fascia during your recovery. Tape applied to the foot serves to take the load off the plantar fascia, this allows the inflammation to reduce and healing to take place.
Medication – Your GP will normally prescribe a non-steroidal anti-inflammatory medication such as ibuprofen, this helps reduce pain and inflammation.
Exercise – Exercises are an important part in your rehabilitation process for plantar fasciitis, and also help to reduce recurrence. A home exercise programme to both strengthen and stretch the muscles of your lower leg and foot is important to ensure that full function returns.
Footwear & orthotics – There are various opinions on footwear and shoe inserts. Some professionals will promote soft supportive shoes with inserts, while others believe that walking barefoot will allow normal foot biomechanics to return. More information about prescription orthotics can be found on the NHS website. Whats best is unique for each patient, your osteopath or allied healthcare professional should discuss your options.
Osteopathy – Osteopathy has been shown to be an effective treatment for a variety of lower limb disorders. The Enfield Osteopath and Enfield Physiotherapy practice can both help speed up your recovery from plantar fasciitis by:
- Increasing the joint mobility in the foot, ankle, knee and hip;
- Reducing muscular and fascial tension in the lower leg and foot;
- Taping to offload and support weight-baring structures;
- Providing a customised home exercise program;
- Personalised advice on activity medication and footwear.
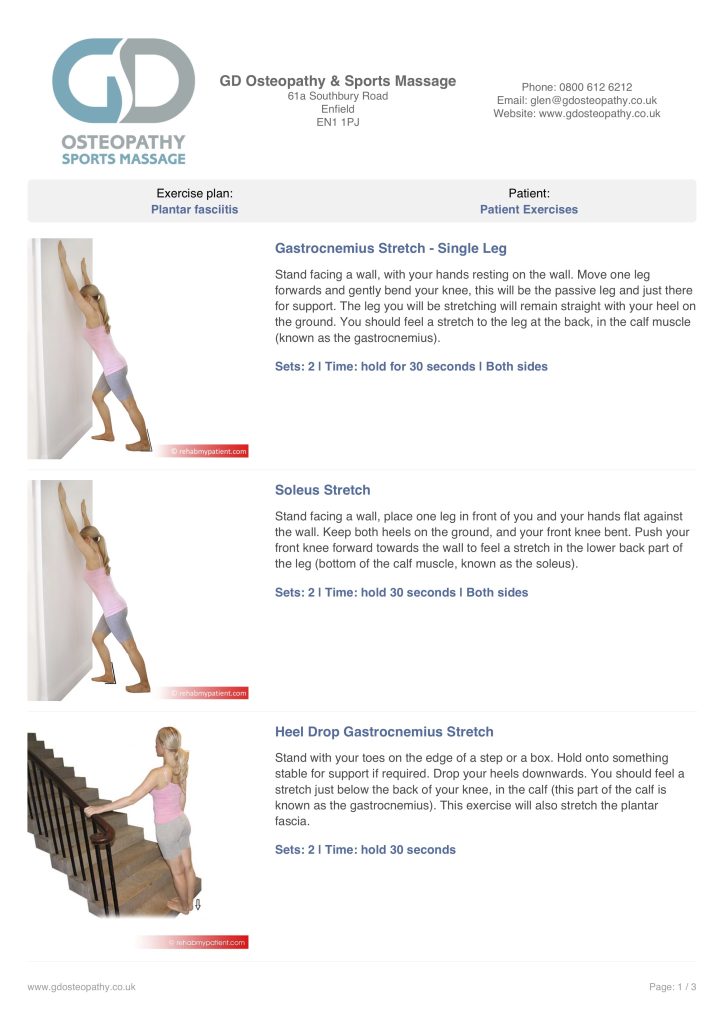
FREE plantar fasciitis exercise plan Click on the link provided or the image below to receive your free planter fasciitis exercise program. It is recommended that this program be used in conjunction and under supervision by one of our osteopaths or sports massage therapists. If you find any of the exercises difficult or painful, please stop and consult your practitioner before continuing.